“How do I know that embryo is really mine?”
This question recently surfaced in the safe space of a patient support group — and once one person voiced it, others quickly followed. Many agreed on how unsettling it can feel to place such trust in what happens behind the closed doors of an IVF laboratory.
Why Patients Worry About Embryo Mix-Ups
Occasionally, news stories emerge from around the world describing cases where the embryo used in treatment did not belong to the intended patient. These incidents represent the worst-case scenario, but their emotional impact travels way beyond the clinic involved. For patients already navigating the physical, emotional, and financial demands of IVF, even the possibility of error can undermine confidence and increase anxiety. So how do fertility clinics protect against this risk?
Human Error and the Origins of Double Witnessing in IVF
Embryologists are highly trained professionals — but they are also human. IVF labs recognised early on that human error is always a possibility, particularly during complex, repetitive procedures performed under time pressure. To reduce risk, clinics introduced double witnessing at critical stages of treatment. In October 2002, the UK regulator — the Human Fertilisation and Embryology Authority (HFEA) — made double witnessing mandatory across all IVF and IUI procedures. This meant that whenever eggs and sperm were mixed, or embryos moved between dishes, two scientists must independently verify patient identity against labels, records, or digital systems.
The Limits of Manual Double Checking
As IVF services expanded and laboratory workloads increased, a new challenge emerged: cognitive overload. A phenomenon known as involuntary automaticity was identified — when people performing repetitive tasks may do so without full conscious awareness. Even with two professionals present, the risk of both missing the same detail or each one relying on the other increases under pressure.
Electronic Witnessing: A Big Leap in IVF Safety
From 2006 onwards, electronic witnessing systems started to be available. These systems use RFID tags or barcodes to electronically link the plasticware that contains egg, sperm or embryos to the correct patient.
How Electronic Witnessing Works
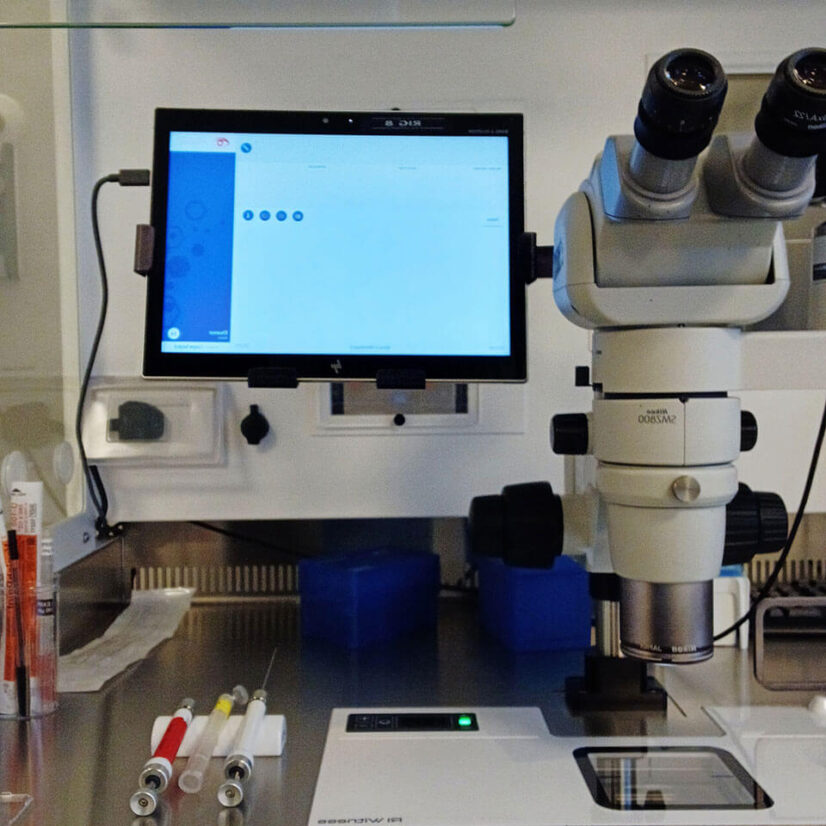
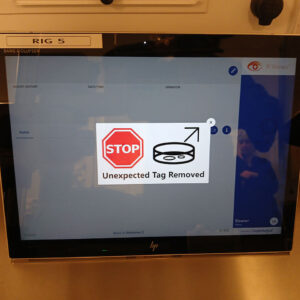
Every piece of lab equipment is assigned to a specific patient – if an unassigned item leaves the work area, an alarm sounds (see image).
If dishes from two different patients enter the same workspace, the system immediately alerts staff; alarms are deliberately disruptive — designed to stop work instantly.
Importantly, manual double witnessing is still required – electronic systems act as an additional layer of protection, not a replacement for human oversight.
Why This Matters for Patients
For patients, electronic witnessing provides something invaluable: traceability and transparency.
An electronic audit trail covers sperm preparation, egg collection, fertilisation checks, embryo culture and transfer. Even frozen embryos are stored in straws labelled with cryogenic-safe barcodes, allowing identity confirmation using handheld scanners at the time of thawing. While no system is ever completely risk-free, modern IVF labs are more reliable and accountable than ever before.
Mistakes can still happen — and clinics must remain open, regulated, and committed to continuous improvement. But today’s IVF labs operate with multiple overlapping safeguards, designed to protect both patients and professionals working under intense pressure. For embryologists, electronic witnessing reduces mental strain and supports sustained focus. Leaving work at the end of the day is easier knowing that everything has been overseen by tech that doesn’t get tired. For patients, it means greater confidence that every possible step has been taken to protect what matters most.